
The aim of this article is to provide a good quality, accurate, easily understandable summary of the details about flea and tick medication poisoning, with a particular focus on the risk of toxicity in cats.
Quick Overview: Flea And Tick Medication Poisoning In Cats





About Flea and Tick Medication Poisoning in Cats
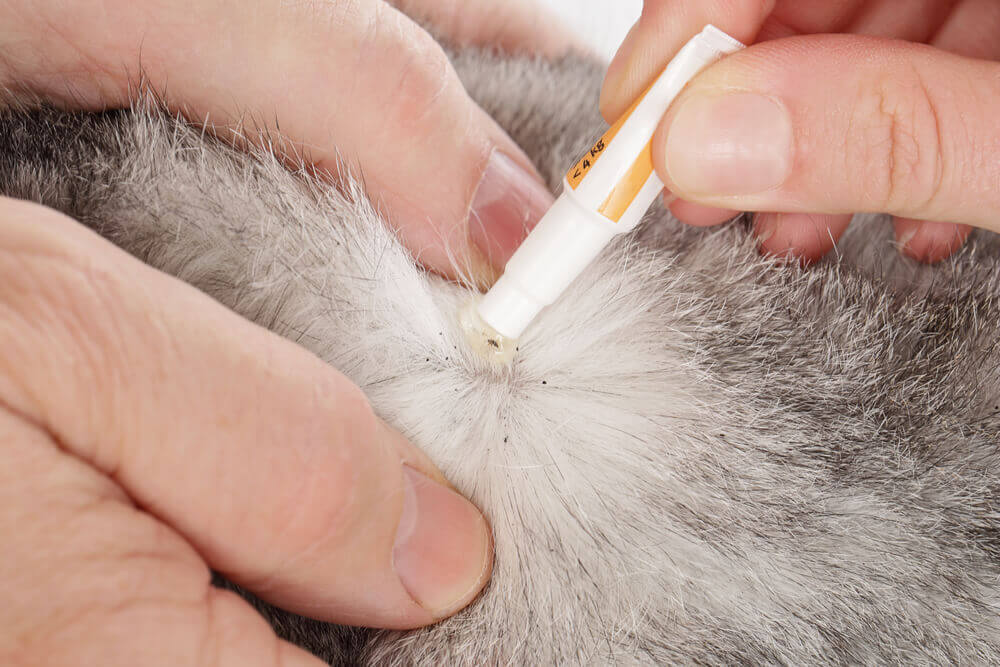
Pet owners often choose to prevent fleas and ticks in cats and dogs using regular medication, which makes sense, but it’s important to remember that the active ingredients of these products can have a toxic effect on cats in certain circumstances.
These products are often available over-the-counter without veterinary supervision, so it’s up to pet owners to read the label carefully to ensure that they use topical flea and tick treatments safely.
While poisoning is unlikely to happen if flea and tick products are used according to manufacturers’ recommendations, mishaps can happen, and it’s common for cats to become ill and even to die following exposure to flea and tick medication when it’s used wrongly.
Exposure may happen via ingestion (e.g. licking spills, or self-grooming chemicals from their own coats) or via absorption (e.g. if a dog flea spot-on product is applied to a cat). It’s important to remember that “cats are not small dogs”: their metabolism works in an entirely different way, making them more vulnerable to certain toxicities compared to dogs.
Toxic reactions are sometimes referred to as side effects, but if the products are used correctly, the risk of side effects is minimal.
What Are the Different Types of Flea and Tick Medication?
Flea and tick medication works in different ways, requiring different specific approaches to toxicity. The most common products are:
- Anticholinesterase Insecticides (organophosphates (OPs) and the carbamates)
- Pyrethrins
- Amitraz
- Isooxazoline antiparasitic agents
The products are available in different formulations, including spot-on topical drops, sprays, powders, and oral medication such as tablets.
Symptoms of Flea and Tick Medication Poisoning in Cats

While poisoning is unlikely to happen if flea and tick products are used according to manufacturers’ recommendations, mishaps can happen, and they can lead to cats becoming ill and even die following exposure to these medications.
The symptoms shown by cats depend on the type of flea and tick medication that they have been exposed to, and they are a consequence of the specific mechanism of action of the particular type of insecticide contained in the product used.
Clinical signs of poisoning include:
- Anorexia
- Salivation (drooling),
- Lacrimation (excessive tear production)
- Diarrhea
- Abdominal cramps and discomfort
- Bradycardia (a slow heart rate), miosis (constricted pupils)
- Frequent urination
Respiratory signs – (difficulty breathing caused by narrowing of the airways and excessive respiratory secretions), as well as muscle tremors and seizures. If left untreated, death can follow, caused by excessive respiratory secretions and/or seizures.
Anticholinesterase Insecticides
These substances (e.g. organophosphates and carbamates) bind to and inhibit cholinesterase, which is an enzyme present in synapses (the connection points between nerves).
They “take out” acetylcholinesterase, leading to an accumulation of acetylcholine (a neurotransmitter) at the junction between the nerve junction, which in turn leads to over-stimulation of the target that is being stimulated by the nerve (e.g. a muscle).
Organophosphates have a stronger and more permanent effect than carbamates but the signs shown by poisoned animals are the same.
Examples of well-known organophosphates (OPs) include:
- Diazinon which may be used in buildings to control infestations of cockroaches, silverfish, ants, and fleas.
- Tetrachlorvinphos which has been used in the past to control fleas and ticks
Pyrethrins
Pyrethrins are a natural substance derived from Chrysanthemum flowers, while pyrethroids are artificially produced synthetic analogues. They act by affecting the sodium channels in cell membranes, leading to prolonged depolarization (stimulation) of nervous tissue.
Most products that are commonly used contain only low levels of pyrethroids, making them toxic to insects but safe for mammals. However spot-on type flea products, containing 45-65% permethrin, are typically used as anti-flea medication in dogs, and although they are clearly labelled for this purpose, they are commonly applied by owners to cats, leading to severe signs of poisoning.
There are several different formulations of products that may contain pyrethrins and it always makes sense to read the label before using any product in a house where there are cats. Examples include allethrin, cypermethrin (CP), deltamethrin, etofenprox and others.
Signs of toxicity include: anorexia, salivation/drooling, agitation and restlessness, hyperthermia, vomiting, incoordination, staggering when trying to jump, walk or even just to stand normally, as well as twitching, trembling and tremoring. In severe cases, there is a risk of death.
Amitraz
Amitraz is an alpha-adrenergic agonist which is used in agriculture, as well as being used to control ticks and Demodex mites in dogs. Poisoning is rare in cats, but again, the use of a dog-specific product in a cat will cause severe toxicity, or if a cat has close contact with a dog that has been treated with amitraz (e.g. sleeping with a dog wearing an amitraz flea collar) this can cause poisoning.
Signs of poisoning include: anorexia, dullness, weakness, incoordination, vomiting, diarrhea, slow heart rate, low body temperature, and potentially death.
Isooxazoline Antiparasitic Agents
These relatively new flea and tick control products (e.g. Fluralaner, lotilaner, serolaner, alfoxolaner) have very low toxicity, but neurologic events (tremors, seizures) have very rarely been reported.
Diagnosis of Flea and Tick Medication Poisoning in Cats

Signs of toxicity include anorexia, salivation/drooling, agitation and restlessness, hyperthermia, vomiting, incoordination, staggering when trying to jump, walk or even just to stand normally.
If your cat has had inappropriate exposure to flea control or anti-tick products (e.g a dog product applied to a cat) or if they are showing signs of being unwell that may be linked to exposure to these products, you should immediately make contact with an emergency veterinarian, as this is a potentially life-threatening situation. In these cases, the diagnosis is obvious, because you know that the exposure has taken place.
In other cases, a cat may present to a veterinarian with signs that are suspicious, and the vet may need to go through a process of making an accurate diagnosis. Contact with the animal poison control centre or the ASPCA poison advice library may be needed to confirm certain details.
Detailed History Taking
Your DVM veterinarian will discuss every aspect of your cat’s life, looking for clues that may include possible exposure to a source of flea and tick medication. Young animals and small animals may be more prone to flea and tick medication poisoning than older, larger cats.
Physical Examination
Your veterinarian will check your cat over carefully, ruling out other causes of the signs that are being shown. A detailed neurological examination will be carried out if your cat is showing signs of a neurological problem, such as twitching or collapse.
Routine Blood Tests and Other Laboratory Work
Your veterinarian may suggest blood tests, including the usual panel of diagnostic tests, such as hematology (complete blood count) and biochemistry profiles, to confirm that there is no other underlying illness affecting your cat.
Urinalysis may also be carried out.
Specialised Tests
The measurement of acetyl choline esterase (ChE) activity in the blood, brain, or retina may be carried out by an external laboratory as a specific diagnostic tool that can be quick and inexpensive.
Treatment of Flea and Tick Medication Poisoning in Cats
General Treatment
The priority initially is to stabilize any general signs of flea and tick medication poisoning:
- Hospitalization for intensive supportive care is often needed, as cats may be seriously unwell
- Respiratory support for cats that are having breathing difficulties
- Anti-seizure medication for a cat that is having seizures
- Anti-emetic treatment to stop vomiting
- Intravenous fluids as general support.
A specific treatment to remove flea and tick medication from the body is often also carried out, to prevent further absorption, with the details depending on the suspected cause.
- Following oral toxicity, vomiting may be induced, gastric lavage may be carried out, activated charcoal may be given, and enemas may be administered.
- Following skin exposure, a cat may be washed in detergent or liquid dish soap to remove all traces of flea and tick medication.
Specific Treatment
As well as the above, specific treatment may be given which depends on the type of flea and tick medication.
- Anticholinesterase insecticides (organophosphates and carbamates)
- Some of the signs of poisoning (so-called muscarinic signs) can be controlled with atropine sulfate, but atropine does not control other signs (e.g. the nicotinic or central nervous system signs). The ideal therapy is pralidoxime chloride (2-PAM), which regenerates acetyl choline esterase by allowing its release from the organophosphate. However this needs to be given at an early stage, as if the organophosphate changes have “aged”, the acetyl choline esterase is permanently attached, and cannot be released.
Intravenous lipid emulsions (ILE) may be suggested as a type of treatment.
Pyrethrins
The signs of pyrethrin toxicity may be controlled using methocarbamol, a muscle relaxant that’s normally used to treat medical conditions that cause acute, painful musculoskeletal spasms. Intravenous lipid emulsions (ILE) have been used successfully in cats with permethrin toxicosis.
Amitraz
A specific drug called yohimbine may be given intravenously to reverse the signs of toxicity. Alternatively, atipamezole (an antidote to sedation that’s in common use in most veterinary clinics) may be administered.
Prognosis
The prognosis depends on the severity of the signs, the type of product involved, and the level of flea and tick medication exposure.
Prevention of Flea and Tick Medication Poisoning in Cats
Fleas like an environmental temperature of 21 – 29’C (70 – 84’F). Fleas are around 3-4mm (1/4 to 1/3 inch)
All insecticides should be used strictly according to the manufacturer’s instructions, and they should be kept out of the reach of cats. Dog parasite control products should never be applied to cats.
Conclusion
Flea and tick medication poisoning is a specific diagnosis linked to exposure to flea and tick medication. Once the problem has been identified, general supportive treatment as well as treatment that’s specific to the type of flea and tick medication can be given.
Frequently Asked Questions
Can cats be poisoned by flea treatment?
As long as flea treatments are used strictly according to manufacturer’s instructions, the risk of cats being poisoned is exceptionally low.
What do I do if my cat ate flea medicine?
You should contact your DVM veterinarian immediately to explain precisely what has happened, with full details of the products involved. They will advise you accordingly.
How long does flea medicine poisoning last?
This depends on how much, of what type, and in what way (skin exposure or ingestion) the cat was exposed to the product. This is a specific question which you should ask the veterinarian attending to your cat.
Is flea and tick medicine poison?
Flea and tick medicine is designed to be poisonous to fleas and ticks, but harmless to cats and other animals, as long as it is used correctly. But yes, it is a type of poison if used incorrectly.
What are the symptoms of flea and tick medication poisoning in cats?
The signs are often non specific, but they often include respiratory, gastrointestinal and neurological signs.
Can cats die from flea and tick medication poisoning?
In severe cases of flea and tick medication poisoning, death is possible, and prompt treatment of poisoned cats is essential.
How long does it take to get flea and tick medication poisoning?
Exposure to high levels of flea and tick medication, or even low levels of certain types of flea and tick medication, can cause rapid signs of toxicity.








What is the best cat flea/tick drops to use ? I use frontline … are there other brands which are less damaging to cats ? or can I use a herb powder ? any advice to get off these drops gladly welcomed. I live in the UK , London.
I would always discuss this with your own vet: there is a wide range of products available now, but availablity varies with location (some products in some countries, not in others). Frontline is fipronil, and there are multiple generic branded versions of this now. It works well, for the right cases, with no evidence of resistance or inefficiency. Herb powders are not generally nearly as effective.
Vets are increasingly asking “does this individual cat need to be on regular flea preventives?” – because not all cats do. It depends on the risk. And this is another reason why this is worth discussing with your vet in person, as they will have a good understanding of your own situation.
You people lie and no nothing about symptoms of flea medication that was sold to me, “revolution Plus”. Of my 3 cats, the on 2 year old siamese female immediately went bezerk running around the house and jumping up on and through furniture like she was a psycho case on LSD from the 60’s. My 9 year old male immediately looked at me with the same look as a hollywood actor, like… “what did you do to me?” The look in his eyes was terrifying enough. He was almost partially paralyzed in the back legs for 2-3 days. I called the company and filed a complaint adverse reaction report. They took all my information about 5 months ago and never heard from them after that. They could care less if your cat recovers or dies. My vet lied to me and said, oh, he has worms, but never showed me the worm and then said I needed flea medication and and wormer for all three with a $250.00 bill. I never wormed the other cats at home and still have no worms. I know they all get kick backs just like doctors for using their drugs and products. It’s criminal. Anything for the love of money. What’s wrong with a flea shampoo? Not dangerous
There is a solid system for reporting and storing all complaints about possible drug reactions: that is how the system works. Even if they do not get back to you individually, the database of possible reactions is there for all to see, and if any trends emerge, appropriate action will be taken.
The truth is that all products licensed for cats have been proven by evidence to be safe and effective in nearly all cases: if this were not so, they would not be granted a licence.
This does not meant that individual reactions never occur: they do, but they are very rare. And they happen with flea shampoos, by the way.
It is not all about “love of money”. It’s about helping cats with safe, effective medications, with the acceptance that very rarely, there may be side effects.