
This article aims to explain the details of fluid therapy for cats. Fluid therapy is a common type of treatment given to cats for many different reasons. This article will summarise the most important aspects of fluid therapy in a way that is easily understood by cat carers.
What Is Fluid Therapy for Cats?
Fluid therapy generally means the administration of sterile fluids to cats, by means of injection using a hypodermic needle. These fluids are needed by cats that are unwell for a range of reasons, listed below. Fluid therapy is one of the most important and effective ways that veterinary medicine is able to treat cats with certain issues.
How Is Fluid Therapy Given to Cats?
There are four ways that fluid therapy can be administered.
1. Intravenous Fluid Therapy
This has to be set up by a veterinarian, and it is the most rapid, effective and direct way to administer fluid therapy. Giving fluids is a key part of critical care in situations where cats are seriously ill.
Vascular access is needed i.e. a way of injecting directly into the bloodstream, which is why this is only carried out by veterinary professionals. An intravenous cannula (or “iv catheter”) is inserted, usually into the cephalic vein (in the front leg), or into the saphenous vein (in the back leg) or occasionally into the jugular vein (in the neck).
The catheter is secured (usually with dressings) and connected to plastic piping that links to a plastic bag containing the sterile fluids (i.e. they are free of all infectious agents such as bacteria, viruses or fungi).
The fluids can be allowed to run into the vein using gravity, but usually the plastic piping is passed through an electricity-powered fluid pump that allows an accurate measurement of the quantity and rate of fluids to be calculated and given.
The fluids are injected directly into the cat’s vein, passing immediately into the bloodstream, and from there into the interstitial fluid, which is the moisture of living tissue, all around the body.
2. Sub-Cutaneous Fluid Therapy
The sterile fluids can be injected directly under the cat’s skin; the usual site of injection is the back of the cat’s neck. The skin here is loose, around the cat’s scruff, and cats generally do not mind injections given in this area.
Sub-cutaneous fluids are slower to reach the bloodstream and then the interstitial fluid compared to intravenous fluids, as the fluids need to be absorbed from the area under the skin into the bloodstream, and this can take several hours. Furthermore, if a cat is dehydrated, the blood supply to subcutaneous areas is poor, and absorption of the fluids may take even longer.
Sub-cutaneous fluid therapy may be used by veterinarians in situations where they are unable to access the animal’s vein (e.g. a fractious animal) and it is often used as part of home-based fluid therapy by owners treating their own cats (e.g. for chronic renal failure). The same type of plastic bag and plastic tubing is used, and this is connected to the hypodermic needle which is injected into the back of the cat’s neck.
The fluid drips through the needle into the sub-cutaneous area by gravity. Alternatively, the fluid may be drawn into a large syringe from the plastic bag, and then directly injected into the sub-cutaneous area.
3. Intra-Osseus Fluid Therapy
Sterile fluids can also be directly injected into the center of a cat’s bones, into the marrow cavity, where it is rapidly absorbed into the circulation. This is almost as effective as intravenous administration, and it is usually used for small animals where it is impossible to set up intravenous access.
A special type of needle needs to be used to inject into the intra-osseus area, and then the fluid may be given by injection from a syringe, or dripped in from the bag.
4. In Theory, Fluid Therapy Can Also Be Given Orally
(E.g. electrolyte solutions given orally to cats when recovering from digestive disorders), but this is not usually included in the general term “fluid therapy”.
Uses of Fluid Therapy for Cats

Fluid therapy is used in cats in any situation where a cat needs extra fluids. The most common conditions that necessitate fluid therapy are:
- Dehydration (with many possible reasons for this, some of which are listed below)
- Chronic renal failure (chronic kidney disease)
- Poisoning
- Gastrointestinal disorders
- Collapse due to many possible causes
- Hypovolemic shock due to many possible causes
- Heat stroke
- Surgery – during and after anaesthesia
- Metabolic crises, such as hypoglycemia or diabetes mellitus
- Resuscitation e.g. after collapse
How Common Is Fluid Therapy?
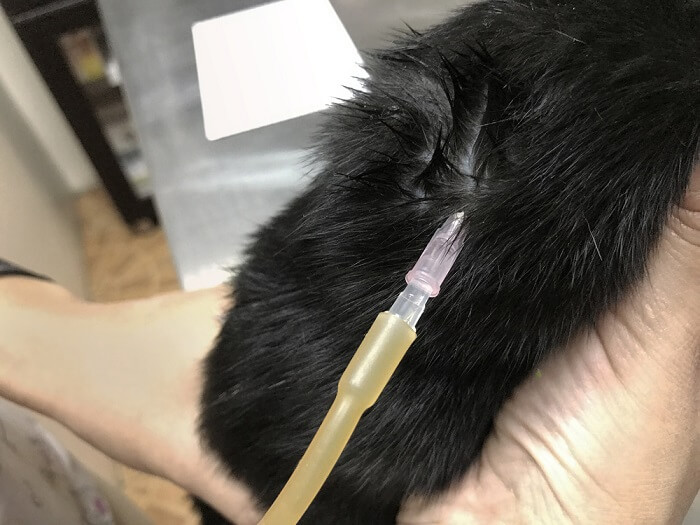
Fluid therapy is very common, being carried out daily in veterinary hospitals for a wide range of reasons. Home-based fluid therapy is carried out increasingly commonly as an adjunct to treatment for chronic renal disease.
How Do Vets Decide That Fluid Therapy in Cats Is Needed?
Your DVM veterinarian will go through a process of decision-making to determine if a cat needs fluid therapy.
1. Detailed History Taking
When you visit the vet with your cat, the vet will discuss every aspect of your cat’s life and health care, obtaining a full background to your cat’s current problem.
This will include questions that relate to your cat’s fluid balance, such as how much your cat is drinking, and any signs that could lead to fluid loss (such as vomiting or diarrhoea), as well as the pattern of urine production.
2. Physical Examination
Your veterinarian will check your cat over carefully, noting any physical signs of illness, and paying particular attention to your cat’s hydration status.
If a cat is severely dehydrated (more than 10%), the skin will “tent” when a fold of skin is gently pinched (i.e. the skin stays in a tent-like position rather than flattening down immediately, as it should do in a normally hydrated cat). The heart rate will be checked.
The mucous membranes (e.g. the gums) will be assessed; these are dry and tacky in a dehydrated cat, due to reduced perfusion with blood. The capillary refill time will be assessed: this gives information about the blood flow to the gums.
Your cat’s body weight will be recorded, as this is an important part of the calculations that need to be done when working out how much fluid needs to be given.
All of these features are repeatedly reviewed by a clinician when a cat is in veterinary hospital being given intravenous fluids.
3. Routine Blood Tests
It’s likely that your veterinarian clinician may also carry out blood work, including hematology (blood count, measuring red blood cells and other aspects) and biochemistry profiles, to find out more about the inner metabolism of your cat.
This often includes a packed cell volume (PCV) which is a useful way of working out a cat’s state of hydration. It’s often used to calculate the volume of fluid needed to rehydrate a cat. This is reviewed with the total protein in the blood, and the albumin level, as a way of making the necessary calculations.
The blood potassium may be measured; in some cases, potassium supplementation is an important part of fluid therapy if a cat’s blood potassium levels are too low. Other electrolytes may also be measured, and the acid-base balance may be assessed.
All of this information is useful when working out what type of fluid needs to be administered, at what rate, and how much.
4. Other Tests
Your veterinarian may measure your cat’s blood pressure. A cat with low blood pressure (hypotension) needs a different amount of fluid to a cat with normal blood pressure.
What Type of Fluid Is Used in Fluid Therapy for Cats?

There are different types of sterile fluids that are used for fluid therapy. They all come in plastic containers: usually in sealed plastic bags, containing 500ml or 1000ml fluid. Sometimes they come in soft plastic bottles instead.
The bags are usually inside an outer plastic bag which has to be opened to gain access to the main bag of fluids. This is torn open manually, like removing the outer packaging from a grocery item. This is to keep the bag of fluids sterile and protected during transit.
The bags have several entrance points at the base, like small protruding nipples. There are two main access points.
- A wider opening that is pierced by the giving set (the tube to carry the fluid to the animal)
- A narrower opening with a flexible plastic/rubber diaphragm that can be used to inject drugs and other substances into the bag of sterile fluids
The bag of fluids has writings on the side that describes what sort of fluids are in the bag: this is like the label on a grocery item, with a description and often a list of ingredients.
The main fluids are known as crystalloid fluids, which means an aqueous solution of mineral salts and other small, water-soluble molecules.
The different types include:
- Normal saline: this is the most commonly used intravenous fluid. It is an isotonic crystalloid solution, containing 0.9% sodium chloride, which is the equivalent of blood without any cells or proteins. This contains only electrolytes and fluid. This is used for simple replacement of standard fluid in situations where an animal may be dehydrated with no other issues.
- Hypertonic saline: this is more concentrated, containing e.g. 3% sodium chloride. This is used in specific clinical situations e.g where fluid needs to be drawn into the circulation from the interstitial spaces (such as edema of the brain)
- A balanced electrolyte solution known as ‘Lactated Ringer’s solution’ or ‘Hartmann’s’ solution. This contains a combination of electrolytes designed to counter some of the metabolic changes seen in cats suffering from issues such as vomiting, certain illnesses, etc.
- Dextrose or glucose is sometimes included in fluids, for situations where an cat may have low blood sugars.
- Synthetic colloids are fluids for intravenous use, and they large molecules, which prolong the time that the fluids remain in the bloodstream. These molecules are usually albumin, a plasma protein, or synthetically modified sugars or collagens. The most frequently used synthetic colloid solutions are hydroxyethyl starch (HES) and gelatin. These are used to expand the fluid in the bloodstream for cats that have lost fluid from the intravascular space in certain situations.
- Whole blood is sometimes used as a type of fluid therapy in certain critical situations where a cat has lost whole blood: this is known as a blood transfusion.
How Do Veterinarians Give Fluid Therapy in Veterinary Hospitals?
The most common fluid to be used at home is either sterile saline, or a balanced electrolyte solution, but your veterinarian will give you clear advice on how to use them.
First, the amount of fluid needed is calculated by your veterinary professionals, and this is based on a number of different factors:
- The illness or situation (see above)
- The presence of hypovolemia (reduced blood volume, e.g. after an episode of bleeding)
- The degree of dehydration
- Ongoing losses of fluids e.g. if a cat is bleeding, vomiting or having diarrhea
- Urine output is also taken into consideration
The veterinarian calculates two important volumes of fluid.
- First, the initial bolus of fluid is to be given to correct the fluid deficit suffered by the cat: this is a relatively large volume that is given more quickly.
- Second, the volume needed to provide for maintenance fluids, based on the normal loss of fluids and need for replacement fluids for a cat.
It’s important to give the correct amount of fluid: if too much fluid is given, as time progresses, there is a serious risk of dangerous fluid overload, where fluid leaks from the bloodstream into the lungs, leading to pulmonary edema, which is a life-threatening complication.
How Do You Give Home Fluid Therapy to a Cat?
Your veterinarian will give you clear advice on how to do this, and the following information is a general guide.
What Fluids Are Used for Home Fluid Therapy?
You can only use the special bag of fluids given to you by your vet for this specific purpose. The fluids used are the same ones that are used in veterinary hospitals intravenous administration.
Your vet will supply you with the correct disposables to give the fluids (bags, tubes, needles, syringes etc.) and will advise you on the amount of fluid to give, how often etc.
The most common fluid to be used at home is either sterile saline, or a balanced electrolyte solution known as ‘Lactated Ringer’s solution’ or ‘Hartmann’s’ solution.
How Is the Fluid Actually Administered?
There are different ways to administer the fluids to your cat.
- The fluid can be given straight from the bag containing the fluid via plastic tubing, attaching this to a hypodermic needle that is injected under the skin. The drip bag is held higher than the cat so that the fluid can trickle under the skin with the help of gravity. It will take 5 – 20 minutes to give the fluid and you need to keep your cat calm for this period: hold them, pet them, or perhaps offer some food.
- Sometimes the fluid may be administered by injection via a large syringe.
It’s best to warm the bag of fluids before administering, by placing it in a bowl of hot water for ten minutes or so. Ideally, they should be lukewarm when injected: this is less likely to cause discomfort than cold fluid.
How Much Fluid Is Given?
Usually, around 10-20 ml/kg of fluid (so 40 -80ml for a typical 4kg cat) can be given, usually in one injection site. When you have finished, you will be able to see this fluid as swelling beneath the skin, like a small cushion.
This fluid will gradually be absorbed into the cat’s circulation, and the swelling will shrink down over a few hours as this happens.
What Do I Do With the Fluid Bag When I Have Finished?
The partly-used fluid bag, the plastic tubes and the needle should be kept in the fridge between different sessions of administration, making sure that you allow them to come back to room temperature before each use by taking out of the fridge an hour or so beforehand.
What Can Go Wrong?
Complications of fluid administration are rare, with the most likely issue being infection or irritation at the injection site, when it will become swollen and painful. If this happens you should contact your veterinarian urgently.
How Much Does It Cost To Treat a Cat With Fluid Therapy?
The cost of fluid therapy includes the disposables needed (needles, intravenous cannula, dressings, plastic tubing, bags of sterile fluids) as well as the use of the equipment (fluid pumps and stands), and the professional time needed to set up and monitor the administration of fluid therapy.
When giving sub-cutaneous fluid therapy at home, the cost of the disposables needs to be covered.
It is impossible to estimate the precise cost, as there are so many possible factors going on in the background of individual cases. You should ask your veterinarian for a detailed estimate before agreeing to proceed with treatment.
However, as a broad indication, fluid therapy in a hospital setting may cost $100-200 to set up, with a similar daily amount for maintenance for as long as it is needed. Home sub-cutaneous fluid therapy may cost $50 to $150 for the equipment and training needed.
Conclusion
Fluid therapy is one of the most valuable tools used by veterinary professionals to treat cats that are seriously ill, and home fluid therapy is a useful extra way of treating cats with chronic renal failure.
Frequently Asked Questions
Do subcutaneous fluids make cats feel better?
If a cat is dehydrated, they feel miserable, a bit like a human with a hangover. Rehydration, by fluid therapy, often makes cats feel immediately more comfortable, and they will start to respond more, being more awake, active and engaging more with their owners.
What does IV fluids do for cats?
Intravenous fluids rapidly correct the fluid balance in a cat's body, correcting dehydration and other imbalances in the metabolism. This can be life saving in many situations, and it also makes cats feel much better.
How long does it take for a cat to feel better after fluids?
A cat will feel better as soon as they are rehydrated, which can be just minutes after intravenous fluids have been given, or hours after subcutaneous fluids have been administered.








Dear Doctor Wedderburn,
I am writing from Petersham, in the State of Massachusetts in the USA.
We live in a rural setting and there is an acute shortage of veterinarians, to the point where long operating clinics are closing leaving owners drives f over an hour for emergency care followed by 4 hour waits.
Our beloved 13 year old Maine Coon Cat is having repeated nasal infections and has been “flushed out” at Angell Vet Hospital in Boston. It is the home of our MSPCA. Great people doing wonderful work.
He is having another round of infections and we are facing a major snow storm this weekend shutting down all facilities. Our cat, Denny Crane, was given a shot of convenia in anticipation of this situation. We are awaiting results of a bacteria culture.
Your website helped us understand this medication and lessened our fears. We realize that Denny may not survive this challenge, but have faith that we are doing all we can.
Thank you for the for the important work you do. God Bless you
Thank you so much for your very kind comments, and I do hope that Denny comes through this. It’s a difficult time and a complex problem.
With my best wishes
Pete
My tabby cat threw up after eating wet food and some greenies. She vomited it all on my bed. She has been vomiting and I felt she was dehydrated. Initially the animal hospital I took her was not even going to give her fluids rushed to judgement that she had kidney renal failure. Honestly I don’t trust their blood work test. I told them she had pancreatitis 1 year and half ago. She got better and she looked very well January 1. Well I’m not sure I was speaking to a vet because this hospital does not allow you to come in with the cat . They asked for 975.00 and I said are you going to do blood work. I gave them the bloodwork of the vet for the last vet. It clearly stated pancreatitis. She stopped eating and urinating and we’ll I said are you going to do anything. They come out to see me if I wanted to resuscitate her for 500 dollars. I said that’s expensive but whatever to save her. But when I took Clarice she was fighting with me to not get into the cat crate bag, she was walking on her own . One of the test showed infection. Her liver was ok and I felt had they provided fluids she would get better. Well since my dog had pancreatitis- I took him to the same place but they stabilized him. I was there over 4 or 5 hours. They did not give her the test for pancreatitis nor PCV to see how much water she loss due to dyhydration. Out of desperation I asked them well thinking they had stabilized her with the fluid I begged them to give her I have no idea if they did that. I mentioned Cernia . Well she said her weight was 2.7 kilograms ( I have some doubts about that ) but she was always a thin cat never heavy. The vet gave her 10 mg /ml) 20 ml injection of Cernia. I know I gave her far less and she got better the last time she vomited and she had no kidney disease . When I returned she was wobbling she could not get out of the bag and could not stand up at all. She stayed on the floor and honestly she looked worse than when I brought her. I thought she may have been sedated . Well an hour later she had a major seizure and I thought she died. I gave her CPR and chest compressions and suddenly she started breathing again but was very weak. She looked terrible. Well I don’t know if what I’m reading is accurate but they say that Cernia injection is given 1 mg or ml per kilogram of weight . They claimed she was 2.7 kilograms. That’s 6 pounds which I doubt. She was 9.8 pounds in 2021. She didn’t look anorexic . She ate every day .
I think 10mg ml of injections of Cernia might have killed her. She certainly was not totally incapacitated when I brought her to them. They gave her Cernia injectable. All I know is that she was in better condition brought in than when released. I am not certain I was even speaking to the vet over the phone Alyssa Carver. My last experience when I brought my dog to them at 1 in the morning who had Cushing disease was also diagnosed as having pancreatitis. But he was overweight and taking the appropriate medication for his condition. The vet was very professional and told me everything they had done explained everything to me did x rays no tumors.
In your opinion do you think that was the appropriate amount of Cernia to a 2.7 kilogram cat suffering from pancreatitis. It was interesting that they did not do that blood test for dyhydration or pancreatitis. They rushed to a conclusion of kidney failure . Her liver was ok.
She died 5 hours later.
Appreciate your opinion. Thank you.
Hello there. The recommended dose of Cerenia is 1mg per 1kg of body weight or 1 ml per 10kg of body weight. Are you sure that the vet gave your cat a full 20ml injection? When vets purchase Cerenia from the supplier, they receive it in 20ml vials, which are certainly not meant to be used in their entirety for a single normal-sized cat. If this is accurate, it would mean that your cat received 200mg of the drug, which is well in excess of the recommended dosage. Is there any way that you can talk with the veterinarian again and confirm the size of the Cerenia dose? I’m sorry for your loss and hope you’re able to find some closure—sounds like a very confusing situation.
Thank you. She needed fluids she was dehydrated so those blood tests would show high levels of BUN and CREATINE just because her electrolytes were so off and had no fluids to eliminate her urine. Vomiting and diarrhea are both signs of dehydration ! She could have been saved if given the right fluids! She went into shock an hour later. I would NEVER recommend that hospital even to my worst enemy. So unprofessional ! Heartless.