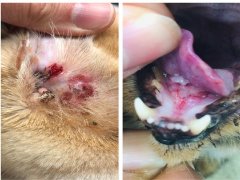
Quick Overview: Stomatitis In Cats
 Urgency: If a cat is in severe pain, they should be seen by a veterinarian as soon as possible, but this is rarely an after-hours emergency.
Urgency: If a cat is in severe pain, they should be seen by a veterinarian as soon as possible, but this is rarely an after-hours emergency.
 Home Remedies: Home dental care is important, using tooth brushing or dental chews to promote optimal oral hygiene, but veterinary care is always needed to tackle the stomatitis itself.
Home Remedies: Home dental care is important, using tooth brushing or dental chews to promote optimal oral hygiene, but veterinary care is always needed to tackle the stomatitis itself.
 Vaccine Available: Vaccines are available against Feline Calicivirus, Feline Herpes Virus and Feline Leukemia Virus, all of which can cause stomatitis, but there are many other possible causes too.
Vaccine Available: Vaccines are available against Feline Calicivirus, Feline Herpes Virus and Feline Leukemia Virus, all of which can cause stomatitis, but there are many other possible causes too.
 Treatment Options: The two main treatment options are first, dentistry, often with multiple extractions of teeth, or second, a medical approach, which can include antibiotics, anti-inflammatory medication, and a range of other possibilities.
Treatment Options: The two main treatment options are first, dentistry, often with multiple extractions of teeth, or second, a medical approach, which can include antibiotics, anti-inflammatory medication, and a range of other possibilities.
 May be Linked to: Feline Immunodeficiency Virus, Feline Calicivirus, Feline Herpes Virus, Feline Leukemia Virus
May be Linked to: Feline Immunodeficiency Virus, Feline Calicivirus, Feline Herpes Virus, Feline Leukemia Virus
 Diagnosis: A physical examination is sufficient to diagnose stomatitis, but it can be complex, expensive and time consuming to diagnose the precise cause, involving blood tests, x-rays, culture of swabs and sometimes biopsies of affected tissue.
Diagnosis: A physical examination is sufficient to diagnose stomatitis, but it can be complex, expensive and time consuming to diagnose the precise cause, involving blood tests, x-rays, culture of swabs and sometimes biopsies of affected tissue.
 Requires Ongoing Medication: Many cases of stomatitis require long term anti-inflammatory medication of some kind.
Requires Ongoing Medication: Many cases of stomatitis require long term anti-inflammatory medication of some kind.
 Common Symptoms: Common clinical signs include halitosis (foul smelling bad breath), difficulty eating (dysphagia), pawing at the mouth, reduced appetite, drooling, bleeding from the mouth, oral pain (e.g. when the mouth is examined), weight loss, and a generally disheveled appearance. Oral tissues lining the mouth appear reddened, swollen and painful, and there may be ulcers.
Common Symptoms: Common clinical signs include halitosis (foul smelling bad breath), difficulty eating (dysphagia), pawing at the mouth, reduced appetite, drooling, bleeding from the mouth, oral pain (e.g. when the mouth is examined), weight loss, and a generally disheveled appearance. Oral tissues lining the mouth appear reddened, swollen and painful, and there may be ulcers.
 Other Names: Feline chronic gingivostomatitis, gingivitis, faucitis, pharyngitis, or a combination of these, depending on precisely which part of the oral cavity is affected.
Other Names: Feline chronic gingivostomatitis, gingivitis, faucitis, pharyngitis, or a combination of these, depending on precisely which part of the oral cavity is affected.
What Is Stomatitis in Cats?
“Stoma” is the Greek word for “mouth”, so stomatitis in cats means “inflammation of the stoma”, “inflammation of the oral cavity”, or “inflammation of the mouth and lips”.
Inflammation causes redness, heat, pain, swelling and loss of normal function, so this is what happens to the lining of a cat’s mouth when stomatitis is present,
Stomatitis is usually a chronic (long term) condition which starts with oral inflammation affecting the gums (the “gingiva”, so it’s “gingivitis”) and gradually extends to include other parts of the lining of the mouth. For this reason, the term “feline chronic gingivostomatitis”, is often used, meaning long term inflammation of the gums and mouth.
Other parts of the oral cavity commonly become inflamed at the same time:
- Faucitis means inflammation of the caudal oral mucosa – the tissue at the back of the mouth behind the premolar and molar teeth.
- Pharyngitis means inflammation of the pharynx, which is the area at the very back of the mouth.
These various expressions all refer to the same basic condition: inflammation of some or all of the mucous membranes that line the oral cavity and upper throat, and in particular, the soft tissues that surround the teeth.
All of the above conditions cause discomfort to an affected cat.
Causes of Stomatitis in Cats
The lining of the mouth comes into contact with a wide number of irritant substances and potential allergens, as well as physically abrasive substances (e.g. in the food or in any objects that are picked up in the mouth and chewed). Any of these can provoke inflammation of the lining of the mouth.
Normally, the body’s defences are able to deal successfully with this challenge, maintaining the lining of the mouth in a healthy state. However sometimes, for a variety of reasons, one of two adverse outcomes may happen.
- An inadequate immune response may allow a pathogen (such as bacteria or viruses) to multiply, causing increased levels of inflammation.
- An over-active immune response may cause significant inflammation to develop in response to an otherwise benign challenge.
The underlying cause of feline stomatitis is often not precisely established, but common causes include the following.
Bacterial Infections
Pathogenic (disease-causing) bacteria are often found in the mouths of cats with stomatitis: these may be a primary cause, or the bacteria may be a secondary complication, aggravating a milder form of inflammation that was initiated by some other primary cause.
Viral Infections

The cat flu viruses commonly cause sneezing, coughing and nasal/ocular discharges in cats, but they are also linked to stomatitis
Feline Calicivirus (FCV) is a common cause of stomatitis in cats, and Feline Herpes Virus (FHV) is also sometimes implicated. Two other viruses, feline leukemia virus (FeLV) and feline immunodeficiency virus (FIV) may also be involved, but their role is not clear, and their impact may be linked more to the fact that they affect the cat’s immune system rather than being involved directly in causing inflammation of the lining of the mouth.
Immune Disease
Inflammation of the lining of the oral cavity sometimes can be a type of immune-mediated or autoimmune disease i.e. an over-reaction of the immune system to normal challenges such as the bacteria and toxins that are found in the build-up of plaque on the teeth (plaque is the sticky semi-liquid film of dissolved food and mucus that gathers on teeth after eating).
If the plaque is left in place, it becomes mineralised, leading to tartar or calculus formation. This is a solid, brown, substance that accumulates, acting as a wider surface area for more plaque to gather on, allowing even more bacteria and toxins to accumulate, aggravating the problem.
Poor dental hygiene is a significant predisposing cause of gingivitis and periodontitis (inflammation of the structures around the teeth) which can then lead on to more widespread stomatitis.
Other Specific Causes
Inflammation of the lining of the mouth can be initiated by a number of other issues, including direct physical irritation (eating irritant materials or some plants), metabolic problems leading to systemic disease (e.g. kidney failure), and immune system failure.
Symptoms of Stomatitis in Cats
Clinical signs of stomatitis include halitosis (foul smelling bad breath), difficulty eating (dysphagia), pawing at the mouth, reduced appetite, drooling, bleeding from the mouth, oral pain (e.g. when the mouth is examined or touched), weight loss, and a generally dishevelled appearance (a cat with stomatitis may suffer discomfort when grooming themselves, leading to an unkempt, poorly maintained coat). When the mouth is inspected, the oral tissues lining the mouth appear reddened, swollen and painful, and there may be ulcers.
The submandibular lymph nodes may be enlarged (lymphadenopathy). The problem is most often seen in mature or middle aged cats, but in some breeds (such as Maine Coon, Siamese, Persian and Abyssinian cats) feline juvenile gingivitis may be seen in cats less than three years of age.
How Does a DVM Veterinarian Approach a Case of Stomatitis?
1. Detailed History Taking
Your vet will discuss every aspect of your cat’s condition and review their overall cat health. There are a number of different possible causes of stomatitis, and this careful history gathering will help to pinpoint the cause.
Many factors are important in this history e.g. senior cats are more prone to certain problems than younger cats, cats that are free-ranging are more prone to some problems than indoor-only cats, etc.
A dietary history is important: what sort of cat food does your cat eat? Has a new food been started recently? Are they being fed any supplements? Are they on any medication? Are there any other factors that could be affecting their digestive system? Is the cat urinating normally? (cat owners should always carefully observe their pet’s behavior in the litter box).
2. Physical Examination
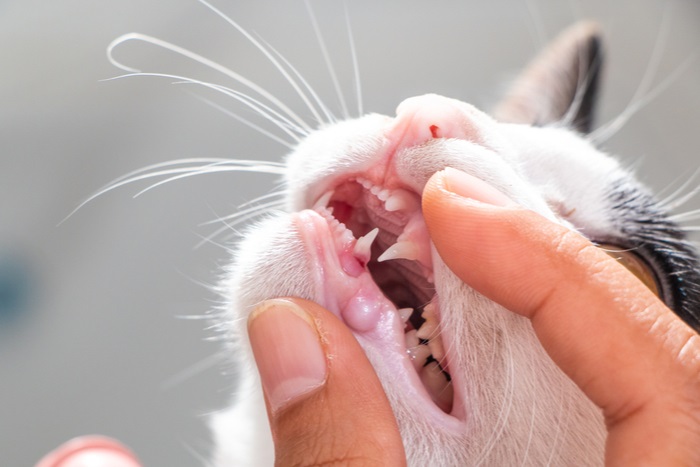
A veterinary examination will involve a close look at your cat’s mouth and teeth
As well as noting the extent of the inflammation in the oral cavity, your veterinarian will check your cat’s body carefully all over, feeling the cat all over, checking for any abnormalities. This will normally include taking the cat’s temperature, listening to their chest with a stethoscope and weighing the cat.
3. Routine Blood and Urine Tests
It’s very likely that your veterinarian may carry out blood work, including the usual panel of diagnostic tests, such as hematology (a complete blood count or CBC) and biochemistry profiles (including liver and kidney enzymes, electrolytes and bilirubin). Simple urine tests may also be carried out.
This type of work up is known as the minimum database, and it’s carried out to review most sick cats, regardless of the signs of illness. The results may provide helpful guidance towards the type of cause of stomatitis.
4. Specialised Blood Tests
Your veterinarian may recommend specific blood tests, such as tests for some viral infections such as Feline Leukemia Virus (FeLV) and Feline Immunodeficiency Virus (FIV), since there are significant implications if your cat is positive for either of these.
5. Additional Tests
If systemic disease of some sort is suspected, general screening tests such as radiography (x-rays) or ultrasound may be recommended.
Dental radiographs (x-rays) may also be taken to evaluate the health of the teeth, and in particular to assess tooth roots and to identify lesions indicating tooth resorption which may indicate that certain teeth may need to be extracted. Dental problems like this are often linked to gingivitis which can then lead to stomatitis.
Culture of swabs taken from the affected areas may be suggested to rule out pathogenic bacteria.
In some cases, a biopsy of the inflamed lining of the mouth may be recommended, to obtain a more detailed understanding of the precise type of inflammation.
6. Referral to a Specialist

Stomatitis can be complex and require input from a veterinary specialist
Rarely, your local veterinarian may recommend referral to a veterinary internal medicine or dental specialist, for an even more detailed review of the diagnosis and treatment of the stomatitis.
How To Treat Gingivitis in Cats
The initial primary aim of a treatment plan is to diagnose the cause of the individual cat’s stomatitis. Only once this has been established can appropriate treatment be organized.
If a cat’s teeth are suspected to be involved, professional dentistry under general anesthesia is often needed, allowing for any necessary tooth extractions, the removal of tartar and plaque, and dental cleaning including polishing of the tooth surfaces. Follow-up home dental care is essential.
Although this sounds extreme, the vet may recommend extraction of some permanent teeth, and sometimes even full mouth extractions, even including the canine teeth. This can sometimes be the only way to resolve severe cases.
This often seems overly radical to cat carers, but the inflammation of the lining of the mouth is often focused at the gum line, which is the junction between the teeth and the gums, relating to the an inflammatory reaction to the plaque build up on the surface of the teeth. If the teeth are removed, the plaque is permanently removed, and the gingivitis often resolves completely.
Medical management of stomatitis is often preferred by cat carers, but this is often not as effective as complete tooth extraction. The risk of side effects from various treatment options should be discussed with your vet.
- Antibiotics may be indicated to resolve any active pathological bacterial component to the problem: common choices include clindamycin, amoxycillin, doxycycline or metronidazole, but your vet will select the most appropriate choice for your cat, and these are not indicated for every case.
- Corticosteroids are sometimes used to alleviate the inflammation: again, they are not always indicated, and this is a decision for your vet.
- Nonsteroidal anti-inflammatory drugs (NSAID’s) are sometimes used for their anti-inflammatory, pain relieving effect.
- Anti-inflammatory medication such as cyclosporine may be used in some cases.
- Omega-interferon given orally or by injection may help to modify the immune response.
- CO2 laser therapy may sometimes be used for specific cases.
- Bovine lactoferrin, applied to the lining of the mouth, may reduce the ability of bacterial pathogens to cause disease in the mouth
- Gold salts, given as intramuscular injections, may help to modulate an over active immune system.
- Stem cell therapy may be used in some cases.
How To Prevent Stomatitis in Cats

Good oral hygiene is recommended for all cats
- A high quality, hypoallergenic diet (with high quality proteins from a low number of sources) may help to reduce the exposure of the oral cavity to irritants and allergenic substances that may initiate inflammation.
- Supplementation with omega 3 and omega 6 fatty acids may decrease the inflammatory response. Topical oral hygiene products that reduce plaque accumulation (e.g. those containing chlorhexidine, or a range of others) may also help.
- A good dental home care regime (e.g. toothbrushing using toothpaste, and/or regular use of dental treats that carry the VOHC seal of approval) is also likely to help by promoting optimal oral health, reducing the incidence of periodontal disease.
Conclusion
Stomatitis is a serious, painful and frustrating disease for cats, their carers and for veterinarians. A detailed work up and a carefully devised treatment plan, with ongoing home dental care, is usually needed to tackle this common problem.
Also Read: Best Dental Cat Treats
Frequently Asked Questions
How long do cats with stomatitis live?
Cats with stomatitis can live a normal length of life, but this does depend on the primary cause of the stomatitis. For example, if the stomatitis is caused by a virus such as FIV, then the cat’s life would be expected to be shorter than normal. In most cases, the stomatitis is not caused by a life limiting condition, which is why most cats have a normal life span. However, the cat’s quality of life can be adversely affected, so this does require careful monitoring to ensure that there is not severe inflammation causing significant suffering.
What is stomatitis caused by in cats?
Possible causes include dental disease, bacterial or viral infections, allergic responses of an overactive immune system, direct physical irritation (eating irritant materials or some plants), metabolic problems leading to systemic disease (e.g. kidney failure), and other, less common causes.
How serious is stomatitis in cats?
Stomatitis is an uncomfortable, often painful condition that affects cats’ mouths. The level of discomfort or pain that is often suffered means that it can be a very serious condition indeed.
Can stomatitis in cats go away on its own?
Stomatitis does sometimes wax and wane in severity, and sometimes as cats grow older, the signs of stomatitis can become less severe. However it rarely goes away entirely on its own, and professional veterinary attention should always be sought.